- Home
- Advice Hub
- Conception
- Trying To Conceive
- How Basal Body Temperature Helps Plan Pregnancy
Basal Body Temperature for Family Planning
Learn how basal body temperature tracking works for family planning, how to chart ovulation accurately and when it helps identify your fertile window.
Whether you are hoping to conceive or looking to avoid pregnancy naturally, understanding your body’s hormonal signals can be a powerful tool. Basal body temperature (BBT) tracking is one of the most widely used methods within fertility awareness, offering a window into your menstrual cycle by reflecting the hormonal changes that occur each month. When interpreted correctly, your BBT chart can help you identify ovulation patterns over time — supporting informed decisions about your reproductive health.
IMPORTANT NOTE: Please be aware that to use fertility awareness methods as a method of contraception, in-depth training from a qualified fertility awareness practitioner is required. This article does not provide you with the information to use this method of natural contraception independently.
What is Basal Body Temperature (BBT)?
Basal body temperature is the body’s lowest resting temperature, measured immediately after waking and before any physical activity, eating, drinking or even talking to your partner! When monitoring your BBT you are looking for a temperature rise that is sustained following ovulation till the end of your cycle, or a temperature that stays elevated, if you conceive.
This shift is driven by progesterone, a hormone produced by the corpus luteum (the casing of the egg) following the eggs release at ovulation. Progesterone has a thermogenic effect, meaning it raises the body’s temperature — a change that, when charted consistently, creates what is known as a biphasic temperature pattern. This two-phase pattern (lower temperatures before ovulation and higher temperatures after) is the foundation of BBT-based fertility tracking.
Research has demonstrated that the post-ovulatory temperature rise, when combined with anther fertility indicator, is a reliable retrospective indicator of ovulation, supporting its use within evidence-based fertility awareness methods (FAMs).
How Basal Body Temperature Reflects Your Menstrual Cycle
Your menstrual cycle is governed by a carefully orchestrated sequence of hormones. BBT responds to these hormonal changes in predictable ways, making it a useful tool for identifying where you are in your cycle.
Follicular phase (before ovulation)
The follicular phase begins on the first day of menstruation and ends at ovulation. During this phase, the pituitary gland releases follicle-stimulating hormone (FSH), which stimulates the ovarian follicles to develop. Oestrogen levels rise as follicles mature, preparing the uterine lining for potential implantation.
During this phase, BBT remains relatively low and stable. Slight daily fluctuations are normal, but there is no consistent upward trend until ovulation occurs.
Ovulation and hormonal changes
Ovulation is triggered by a surge in luteinising hormone (LH), which causes the dominant follicle to rupture and release a mature egg. This is the most fertile point in the cycle; the egg remains viable, and therefore available for fertilisation with sperm, for approximately 12–24 hours.
Following ovulation, the ruptured follicle transforms into the corpus luteum, which begins producing progesterone. It is this progesterone surge that causes BBT to rise.
Luteal phase (after ovulation)
Once ovulation has occurred, BBT typically remains elevated for the remainder of the cycle — usually around 10–16 days. A sustained temperature rise of at least 0.2°C above the coverline (see the charting section below) for three consecutive days is generally considered confirmation that ovulation has taken place, if the preceding six temperatures have remained below the coverline.
If pregnancy does not occur, progesterone levels drop, the uterine lining sheds, and BBT falls back to baseline as a new cycle begins.
How to Track Basal Body Temperature Accurately
Accurate BBT tracking requires consistency above all else. Even small deviations in method can affect the reliability of your chart. Follow these steps for the most dependable results (but remember if you are using FAM’s to avoid pregnancy get in-depth training from a qualified practitioner and do not rely on this article).
Step 1: Measure temperature at the same time every morning
Take your temperature immediately upon waking — before sitting up, drinking, eating, or going to the bathroom. Even mild physical activity can elevate your reading. Aim to measure at the same time each day, as sleeping later or earlier than usual can affect results. A variation of more than 30 minutes from your usual wake time should be noted on your chart.
Step 2: Use a Basal Body Temperature thermometer
Standard oral thermometers may not be precise enough for BBT tracking. A dedicated basal thermometer measures to two decimal places (e.g. 36.54°C), providing the granularity needed to identify the small shifts that signal ovulation. Both oral and vaginal thermometers are available; whichever route you choose, use the same one consistently throughout your cycle. You may choose to use a fertility monitor, and many are available to suit your needs and budget.
Step 3: Record Readings Daily
Record your temperature every morning without exception, even during menstruation. Tracking options include:
- Paper fertility charts (available from Fertility UK)
- Digital apps such as Read Your Body
- Wearable devices that measure temperature automatically overnight such as the Ultrahuman Ring and their Cycle and Ovulation Pro powerplug
Whichever when you choose, take your time to do your research. If you are choosing an app or a wearable, make sure these are back by robust research like the suggestions above.
When recording, note any factors that may affect your reading, such as illness, alcohol consumption, a disrupted night’s sleep, or travel across time zones.
Step 4: Keep tracking
Patterns become far more meaningful over multiple cycles, and whilst it might be tempting to stop charting after a few cycles, don’t. Many factors such as sleep disturbance, illness, medication etc can influence and change our cycles, it is important to always chart.
Step 5: Add in another indicator
Temperature tracking using BBT can become even more reliable if you add in a second indicator such as cervical mucus or cervical position changes. You can find out more about these two indicators and how to monitor and record them here.
Understanding Your BBT Chart
Many people begin BBT tracking without fully understanding how to read their chart. This section covers the key concepts that turn raw data into meaningful insight.
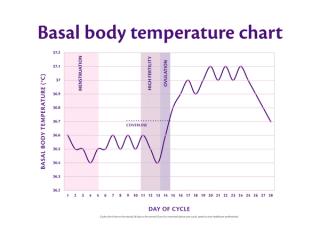
The biphasic pattern
A typical BBT chart displays two distinct temperature phases: a lower phase before ovulation and a higher phase after. This biphasic pattern is the hallmark of an ovulatory cycle. If your chart remains monophasic (temperatures stay roughly the same throughout the cycle), this may suggest that ovulation did not occur — a condition known as anovulation, which can have various causes and is worth discussing with a healthcare professional. You may also notice cycles longer or shorter than 28 days. This may be normal for you but could also indicate conditions such as PCOS (https://www.hipp.co.uk/advice/conception/fertility-and-infertility/getting-pregnant-with-pcos) or, in the case of short cycles, perimenopause. If you are at all concerned about your cycle length, speak with your doctor.
The coverline
The coverline is a horizontal reference line drawn on your chart to help identify the temperature shift. It is typically set above the highest temperature recorded during the last six days of the follicular phase (before the rise). When your temperature rises above the coverline and stays there for three consecutive days, ovulation is considered confirmed. If you are using an app or device, the coverline will be included in the graph you see.
Recognising temperature shifts
Look for a clear, sustained rise rather than a single high reading. One elevated temperature could be due to illness or a disrupted sleep pattern. A genuine post-ovulatory shift is consistent and remains elevated until your next period.
Irregular patterns and what they may mean
Not every chart follows a textbook pattern. Common variations include:
- A slow, gradual rise rather than a sharp shift — still valid, but harder to pinpoint.
- A ‘fallback’ reading one to two days after the initial rise — common and usually not cause for concern. This means ovulation has not happened as yet.
- Very late ovulation (e.g. day 21 or later) — particularly common after stopping hormonal contraception or in women with PCOS
- No clear biphasic pattern — may indicate anovulation, especially if persistent. Common for women suffering with PCOS, other ovulatory disorders or stress.
It is important to remember that BBT confirms ovulation retrospectively. It tells you that ovulation has already occurred, not that it is about to happen. This distinction is critical when using BBT for contraception. If you need to understand when your ovulation is predicted, you may like to see if the device OvuSense is for you.
Using Basal Body Temperature When Trying to Conceive
For those hoping to become pregnant, BBT tracking offers valuable information about the timing of ovulation — which in turn helps identify the fertile window.
Sperm can survive in the female reproductive tract for up to five days under favourable cervical mucus conditions, meaning the fertile window extends before ovulation, not just on the day itself. Because BBT only confirms ovulation after the event, it is most useful for identifying your typical ovulation timing across multiple cycles, helping you predict when to time intercourse in future cycles.
Combining BBT with cervical mucus observation significantly improves accuracy. Fertile-quality cervical mucus — clear, slippery, and stretchy, often described as resembling raw egg white — typically appears in the days leading up to ovulation. Together, these signs form the basis of the Sympto-Thermal Method (STM), one of the most well-researched fertility awareness approaches.
Using Basal Body Temperature to Avoid Pregnancy
BBT also forms part of natural family planning (NFP) methods used to avoid pregnancy without hormonal contraception. However, it is essential to understand both how this works and its limitations and to work with a qualified fertility awareness practitioner to understand the method effectively and ensure it is applied correctly.
BBT alone is considered insufficient for reliable contraception. The Faculty of Sexual and Reproductive Healthcare (FSRH) notes that fertility awareness methods are most effective when multiple signs are combined. Used in isolation, BBT has a higher failure rate than when it is integrated into a comprehensive approach such as the Sympto-Thermal Method, which incorporates another indicator and cycle length data.
Factors That Can Affect Basal Body Temperature
A number of everyday factors can influence your BBT reading, producing apparent outliers on your chart. Recording these alongside your daily temperature helps you interpret your data accurately and avoid misreading a genuine ovulatory shift.
- Illness or fever: Any infection causing a fever will elevate BBT independently of hormonal changes. Mark these readings clearly on your chart.
- Disrupted or insufficient sleep: BBT rises if you have had fewer than three consecutive hours of sleep before taking your reading, or if your sleep has been significantly disrupted.
- Alcohol consumption: Even moderate alcohol intake the night before can elevate the following morning’s reading.
- Travel and time zone changes: Crossing time zones disrupts your circadian rhythm and can temporarily affect your temperature pattern.
- Certain medications: Some drugs — including antihistamines and certain antidepressants — may influence BBT. Speak to your GP if you are unsure.
- Breastfeeding: Prolactin, the hormone that supports milk production, can suppress ovulation and disrupt typical temperature patterns in the postpartum period.
When any of these factors are present, mark the reading as potentially unreliable. Most charting apps and paper charts include a notes field for this purpose. A single reading should not be used to draw conclusions about ovulation.
Basal Body Temperature vs Other Fertility Tracking Methods
BBT tracking is just one of several tools available for fertility awareness. The table below compares the most used methods to help you understand how they work together.
| Method | What it measures | Predicts or confirms? | Limitations |
|---|---|---|---|
| BBT Tracking | Post-ovulatory temperature rise | Confirms ovulation retrospectively | Requires consistency; affected by sleep, illness, alcohol |
| Ovulation Predictor Kits (OPKs) | LH surge in urine | Predicts ovulation 24–36 hours ahead | Cost; LH surges can occur without ovulation (e.g. in PCOS) and are therefore inaccurate for these women |
| Cervical Mucus Observation | Changes in vaginal discharge | Predicts fertile window | Requires practice; can be affected by infections or medications |
| Fertility Apps | Algorithmic cycle prediction | Predicts based on past cycles | Less accurate for irregular cycles; some use BBT and mucus data |
| Devices and Wearables | Algorithmic cycle prediction | Most only confirm and predict based on past data. OvuSense and Ultrahuman C&O Pro predict and confirm based on real time data | Higher cost; Some more accurate than others, especially if using CBT as opposed to BBT. |
Is Basal Body Temperature Tracking Right for You?
Advantages
- Natural and hormone-free — no side effects
- Low cost (unless investing in a monitor or wearable)— a basal thermometer and a chart or app is all you need
- Builds deeper awareness of your menstrual cycle and hormonal health
- Can help identify potential hormonal irregularities worth discussing with a GP
- Compatible with a wide range of fertility goals, from conception to natural family planning (with training)
- Use of a monitor or device is less onerous on the individual and provides greater accuracy in some cases
Limitations
- Requires daily consistency (BBT recordings using a thermometer) — missed readings affect chart accuracy
- Confirms ovulation only after it has occurred (unless using a method able to predict ovulation), limiting usefulness for predicting the fertile window in real time
- Can be more difficult to interpret with irregular sleep patterns, shift work, or postpartum cycles
- Not recommended as a standalone contraceptive method without proper training and the use of a secondary indicator
- May be less reliable during perimenopause, when hormonal fluctuations are less predictable
If you have very irregular cycles, a recent history of hormonal contraception, are going through the perimenopause/menopause or underlying conditions such as PCOS or thyroid disorders, speak to a GP or fertility specialist before relying on BBT tracking alone for contraception or conception planning.
Conclusion
Basal body temperature tracking is a well-established, evidence-based tool for fertility awareness. By monitoring the subtle temperature shifts driven by progesterone, it is possible to identify retrospective ovulation and — over time — build a clearer picture of your cycle’s unique patterns.
Some monitors and wearables, such as those using CBT and providing predictions of ovulation offer greater reliability and convenience.
Whether you are trying to conceive , explore natural family planning, or simply better understand your reproductive health, tracking your temperature offers a hormone-free means of connecting with your body’s natural rhythms. For best results, combine it with other fertility signs, track consistently across multiple cycles, and seek guidance from a healthcare professional or qualified fertility awareness educator if you have any concerns or wish to use this method as your contraception.
Frequently Asked Questions around BBT
The best time to take your BBT is immediately upon waking — before getting out of bed, drinking, eating, or any physical activity. Aim to measure at the same time each morning for consistency. If you wake significantly earlier or later than usual, note this on your chart as it may affect the reading.
Everyone is different however, after ovulation, BBT typically rises by approximately 0.2–0.5°C (0.4–0.9°F) above your pre-ovulatory baseline. This rise is caused by progesterone produced by the corpus luteum and is sustained for the remainder of the cycle.
BBT cannot predict ovulation in advance — it can only confirm that ovulation has already occurred. The temperature rise happens after the egg has been released.
As cycles can vary from month to month, it is recommended that you continue to track each cycle. However, if you are only using BBT to help achieve pregnancy then 3-months if tracking will give you a good idea of when you tend to ovulate. Ideally though, track every month if you can.
Yes. Both illness and disrupted sleep can elevate BBT independently of hormonal changes, producing misleading readings on your chart. If you are unwell, have had fewer than three consecutive hours of sleep before taking your temperature, or have consumed alcohol the evening before, mark the reading as potentially unreliable and do not use it to draw conclusions about ovulation.





