- Home
- Advice Hub
- Pregnancy
- Pregnancy Symptoms & Issues
- Severe Vomiting In Pregnancy (Hyperemesis Gravidarum)
Understanding Severe Vomiting in Pregnancy: A Guide to Hyperemesis Gravidarum (HG)
Learn about Hyperemesis Gravidarum, the severe form of pregnancy vomiting. Discover symptoms, causes, treatment options and expert tips for managing this condition.
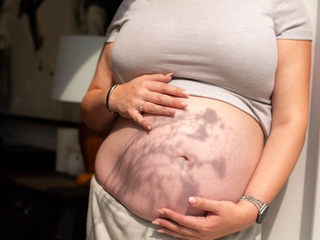
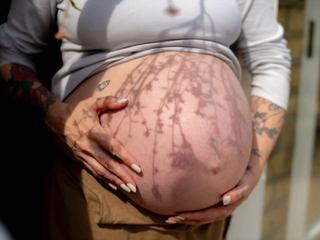
Morning sickness is often thought of as nothing more than a little nausea when you first wake up in the morning and at worst will last for a few weeks. However, for some expectant mums, this is a far cry from reality. Contrary to common beliefs, morning sickness is not just confined to mornings, and it can last well beyond a couple of weeks. If you are struggling with keeping food or water down and are unable to carry on with basic daily activities because of nausea and/or vomiting, it's possible you have a condition known as Hyperemesis Gravidarum (HG).
At HiPP Organic, we believe that understanding your body is the foundation for a healthy, happy pregnancy. This article will give you an evidence-based insight into severe vomiting in pregnancy, helping understand the difference between common symptoms that shouldn’t cause worry, from those that require medical treatment.
Medical Disclaimer: This information is solely for educational purposes and is not a substitute for professional medical advice, diagnosis, or treatment. Always seek the advice of your GP, midwife, or other qualified health provider with any questions you may have regarding a medical condition.
What is Hyperemesis Gravidarum?
Hyperemesis Gravidarum (HG) is nausea and vomiting in its most severe form, occurring during pregnancy. It bears no comparison to regular morning sickness.
HG is a recognised medical condition in which women experience nausea and vomiting so extreme that it leads to dehydration, weight loss, and electrolyte imbalances.
HG is a debilitating condition affecting approximately 1% to 3% of pregnancies and often requires medical treatment to ensure the wellbeing of both mum and baby.
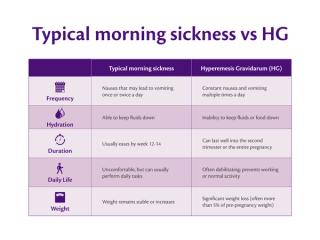

Symptoms and Signs of HG
HG usually presents between the 4th and 6th week of pregnancy.
Being able to recognise the signs early is crucial for managing the condition before it leads to severe physical and mental depletion
Key symptoms include:
- Persistent Nausea: A "never-ending" feeling of sickness that does not go away after vomiting.
- Severe Dehydration: urine will be dark in colour, urination will be infrequent and volumes will be small, extreme thirst, and dry skin and mouth.
- Physical Weakness: Feeling faint, dizzy and lightheaded.
- Weight Loss: A loss greater than 5% of your total body weight.
- Sensitivity to Smells: An extreme aversion to odours that can trigger immediate vomiting.
Causes and Risk Factors
We don't yet fully understand the exact cause of HG, however, some studies suggest that there is a link with the rapidly rising pregnancy hormones, namely human chorionic gonadotropin (hCG) and oestrogen.
A genetic link has also been identified, specifically involving the hormone GDF15, which is thought to influence the brain's "vomiting centre."
There is a higher chance of developing HG during a first pregnancy, when carrying multiples (twins or triplets), or have a family history of HG (your mother or sister) or experienced HG in a previous pregnancy.
Complications of Untreated HG
If left untreated, HG can lead to dehydration, causing low potassium and sodium (electrolyte imbalances), which can affect heart and kidney function.
Not being able to keep food down can lead to a Vitamin B1 deficiency, which increases the risk of neurological problems, in very extreme and rare cases.
For babies, untreated HG can lead to a lower birth weight or a premature birth. However, with timely diagnosis and the correct treatment, these risks are largely minimised.
How is Hyperemesis Gravidarum Diagnosed?
Diagnosis of HG is largely based on your clinical history and presenting symptoms. Your Midwife or Doctor will review how often you are vomiting, your ability to keep food down, and observe for signs of dehydration, such as dark urine and a raised heart rate.
They will carry out urine tests and check for the presence of ketones (a byproduct of the body using fat for energy as opposed to glucose). Blood tests will be taken to check electrolyte levels and organ function. Lastly, they will perform an ultrasound to check for multiples such as twins or triplets or other underlying causes.
Treatment and Management Options
Depending on the severity of HG, treatment options can be as simple as lifestyle adjustments or as serious as requiring a hospital admission for medical treatment.
Supportive home strategies
If the HG symptoms are reasonably mild, lifestyle changes such as eating more frequent, smaller meals, which are low in fat and high in carbohydrates, can provide some relief from symptoms.
Dry toast and plain biscuits are great examples of tolerable high carbohydrate and low fat food options. Avoiding triggering odours and sipping ginger tea can provide light relief also. Sucking on ice cubes is often easier than drinking a glass of water.
Medical interventions
When lifestyle changes don't quite cut it (and they often don't), there are many medical treatments available to help manage the symptoms such as: anti sickness medications that are safe for use in pregnancy, rehydration with fluids through an IV drip and supplementation with B-vitamins to prevent deficiencies. In more extreme cases, a stay in hospital may be necessary to treat severe nausea, vomiting and dehydration.
Living with HG: Coping and Support
Experiencing HG is both physically and mentally exhausting. It is common to feel dismissed, isolated and exhausted. It is important to communicate with your employer and midwife/doctor as soon as you feel the symptoms are getting out of hand.
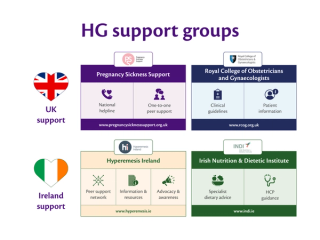
HYPEREMESIS GRAVIDARUM (HG) SUPPORT GROUPS: IRELAND & UK
IRELAND SUPPORT
Peer support network, information, resources, and advocacy.
Irish Nutrition & Dietetic Institute (INDI)
Specialist dietary advice and healthcare professional (HCP) guidance.
UK SUPPORT
Pregnancy Sickness Support (PSS)
National helpline, one-to-one peer support, and online forums.
Royal College of Obstetricians and Gynaecologists (RCOG)
Clinical guidelines, research, and patient information leaflets.
***Consult your midwife or GP for personalised medical advice and referrals.
Prognosis and Outlook
HG usually improves significantly by the 16th to 20th week of pregnancy. However, there are still a very small cohort of women who will continue to have symptoms right up until the birth of their baby. With the right medical treatment, most pregnancies have a healthy and positive outcome. Symptoms disappear almost immediately once the baby is born.
When to Seek Medical Help
You should contact your Midwife, Doctor, GP or local maternity unit immediately if you experience any of the following symptoms: Unable to keep any food or fluids down for 24 hours, not passing urine for more than 8 hours, passing urine that is dark in colour, losing weight quickly, having tummy pains, developing a high temperature or feeling faint or dizzy when standing up.
FAQs around HG
If you are vomiting so often that it's causing you to lose weight, becoming dehydrated, and is stopping you from being able to go about your normal activities of daily life, it is likely that you have HG and not the regular morning sickness.
For most, symptoms are at their most severe from the 9th to the 12th week of pregnancy and tend to subside by the second trimester. However, a small percentage of women can continue to have symptoms and require treatment right up until the birth of their baby.
The main risks are dehydration, electrolyte imbalance, and weight loss. With medical treatment, these are typically managed with good effect and don't cause any long term harm to mum or baby.
HG is relatively rare, affecting approximately 1 to 3 out of every 100 pregnancies.
Generally, if a HG pregnancy is appropriately managed and you can tolerate some food and hydration, your baby will be perfectly healthy. It's only if HG is left entirely untreated that the main risks (prematurity and low birth weight) can occur.